Blog
Loop conization
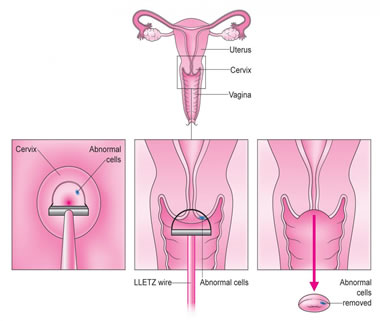
Conization is a diagnostic and therapeutic procedure in which a diseased part of a cone-shaped cervix is cut off with a radio-wave surgical knife. It is very important that all pathological changes are within the cone base.
The depth and width of the cone is determined except by Schiller's trial or colposcopic findings and by the patient's age, as well as by reproductive history (number of births). As a rule, the cone is shallow and wide bases in younger patients. In older patients, the cone may have a narrower base, but the length of the cone is longer - up to the inner mouth of the cervix. The resulting cone is fixed in formalin and referred to the pathologist. Only in this way can the grade of neoplasia be evaluated (CIN I, II, III). In this procedure, the most important thing is that the edges of the cone are free from pathological changes, then conisation is the final therapeutic procedure. If the pathological change affects one of the edges of the cone, treatment is not complete. Rehab or hysterectomy should be performed, depending on the patient's age and birth preference. Classical conization involves the removal of the diseased part of the cervix with a surgical knife - scalpel, which is why it is called surgical conization. Reconstruction of the cervix after surgical conization is performed by circular suturing of the cervix, which almost always leaves minor or major deformity of the cervix.
Recently, a very popular method of conization called electrosurgical resection of the cervical transformation zone with the help of a high frequency current called LEEP (Loop Electrosurgical Excision Procedure). The advantages of this technique are the ease of surgery, shorter surgery time, the possibility of performing an intervention in local anesthesia, as well as less postoperative problems. Early complications of conization are subsequent bleeding (4%), which most commonly occurs 5. days after the intervention. Bleeding may also occur 10 days after the intervention. By its nature, this bleeding cannot endanger the patient. Preparing a pacifier for intervention involves abstinence from eating and drinking for at least 5 hours, performed a PAPA test, colposcopic examination, bacterial examination of the vaginal and cervical swabs. The intervention is performed in the outpatient setting under local anesthesia or short-term intravenous sedation - anesthesia, and the patient's retention time is up to 2 hours.
Colposcopy
It is a method of observing the vulva, vagina and cervix with the help of a colposcope. A colposcope is an optical instrument with a magnification of 5 - 30 times. The accuracy of diagnosis by this method is between 60 - 85%, and in combination with the PAPA test is 98 - 99%. Simple or native colposcopy means simple observation of the cervix and extended colposcopy involves the use of chemical and optical aids. One of the optical aids is a green filter that can better see blood vessels on the surface of the cervix. The chemical aid is 3% acetic acid and Lugol's solution. Under the influence of acetic acid, the cylindrical epithelium of the kidney I becomes "anemic" and the cellular proteins are denatured, which is referred to as the aceto-white reaction. Applying Lugol's solution (Schiller's probe) to the surface of the squamous-layered epithelium, glycogen in the superficial cells binds iodine and the epithelium itself stains to a dark brown color - an iodine positive reaction. An iodine positive reaction with a certain degree of certainty precludes the existence of epithelial atypia.
 34
34
 1500
1500
 5
5